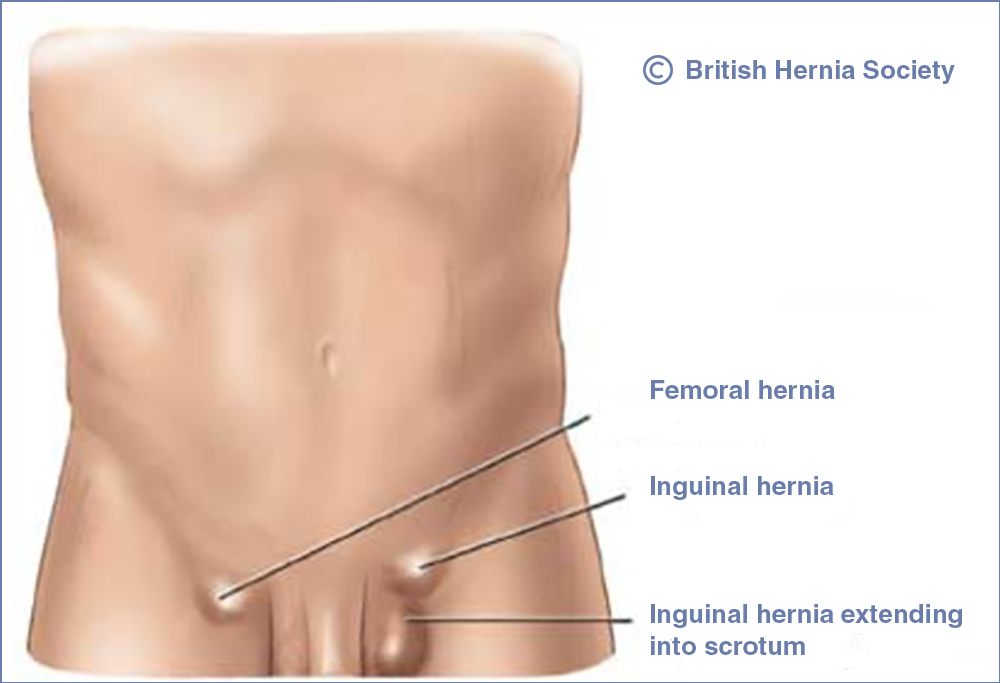
A hernia occurs when an internal part of the body pushes through a weakness in the muscle or surrounding tissue wall. It usually develops between your chest and hips. In many cases, it causes no or very few symptoms, although you may notice a swelling or lump in your tummy (abdomen) or groin.
The lump can often be pushed back in or disappears when you lie down. Coughing or straining may make the lump appear.
Other types of hernia that can affect the abdomen include:
- incisional hernias – where tissue pokes through a surgical wound in your abdomen that hasn’t fully healed
- epigastric hernias – where fatty tissue pokes through your abdomen, between your navel and the lower part of your breastbone (sternum)
- spigelian hernias – where part of your bowel pokes through your abdomen at the side of your abdominal muscle, below your navel
- diaphragmatic hernias – where organs in your abdomen move into your chest through an opening in the diaphragm; this can also affect babies if their diaphragm doesn’t develop properly in the womb
- muscle hernias – where part of a muscle pokes through your abdomen; they also occur in leg muscles as the result of a sports injury
Your GP or consultant will usually be able to identify a hernia by examining the affected area. A number of factors will then be considered when deciding whether surgery is appropriate, including:
- the type of hernia – some types of hernia are more likely to become strangulated, or cause a bowel obstruction, than others
- the content of your hernia – if the hernia contains a part of your bowel, muscle or other tissue, there may be a risk of strangulation or obstruction
- your symptoms and the impact on your daily life – surgery may be recommended if your symptoms are severe or getting worse, or if the hernia is affecting your ability to carry out your normal activities
- your general health – surgery may be too much of a risk if your general health is poor
There are two main ways surgery for hernias can be carried out:
- open surgery – where one cut is made to allow the surgeon to push the lump back into the abdomen
- keyhole (laparoscopic) surgery – this is a less invasive, but more difficult, technique where several smaller cuts are made, allowing the surgeon to use various special instruments to repair the hernia
Most people are able to go home the same day or the day after surgery and make a full recovery within a few weeks.